The shoulder is one of the most complex and mobile joints in the human body. A common and important question patients ask is, “Can you get rheumatoid arthritis in your shoulder?” The answer is yes, and for many individuals living with this chronic autoimmune disease, the shoulder joint can become a significant site of pain. Understanding how rheumatoid arthritis (RA) affects the shoulder is the first step toward management. In this post, we’ll explore the connection between RA and shoulder pain, detailing the symptoms, diagnosis, and treatment options available.
Key Takeaways
- Rheumatoid arthritis is an autoimmune disease where the body’s immune system mistakenly attacks the synovium, the lining of the joints.
- The primary joints affected in the shoulder are the glenohumeral joint (the main ball-and-socket) and the acromioclavicular (AC) joint.
- Symptoms often include bilateral pain and stiffness, warmth, swelling, and a grinding sensation (crepitus), typically worse in the morning.
The Shoulder Joint: A Primer on Complex Anatomy
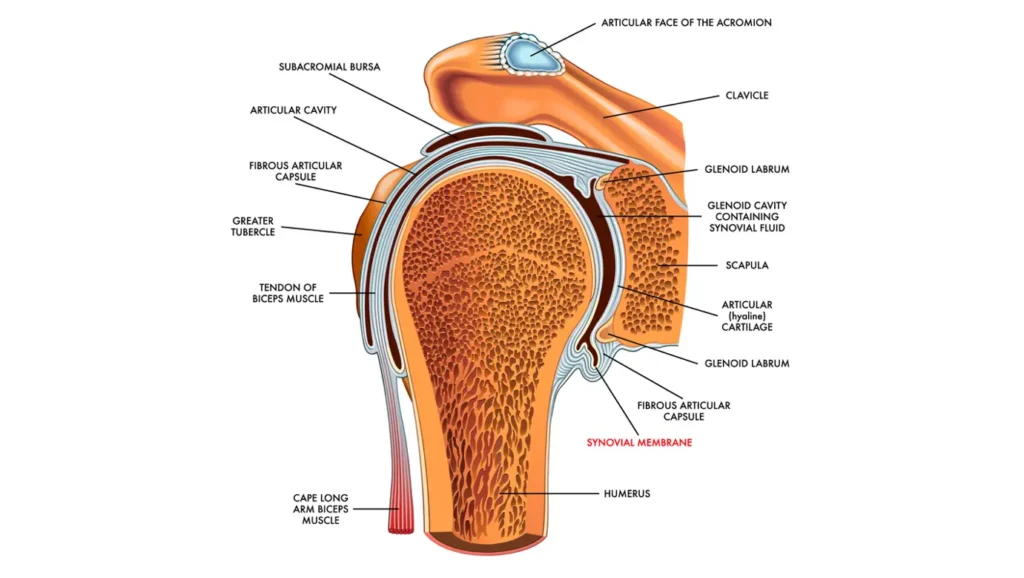
The main joint of the shoulder is the glenohumeral joint. This is a classic ball-and-socket joint. The head of the humerus (the upper arm bone) fits into the glenoid, a shallow socket on the shoulder blade (scapula). The shoulder also includes the acromioclavicular (AC) joint, which is where the collarbone (clavicle) meets the shoulder blade (acromion).
Both joints are lined with a thin membrane called the synovium. The synovium produces synovial fluid. This fluid lubricates the joint to support smooth, frictionless movement. Surrounding the joint is the rotator cuff, a group of four muscles and their tendons, which provide stability and allow you to lift and rotate your arm.
Can You Get Rheumatoid Arthritis in Your Shoulder?
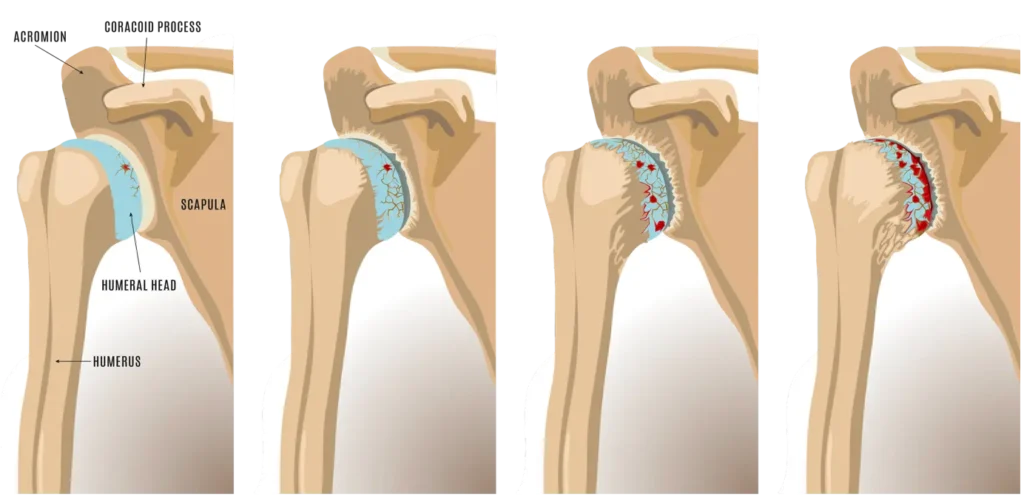
Yes, you absolutely can get rheumatoid arthritis in your shoulder. This condition is a systemic autoimmune disorder. Rheumatoid arthritis often begins when the immune system malfunctions. It incorrectly identifies the synovium as a foreign threat, and the body then launches an inflammatory attack against this healthy tissue. This process is called synovitis. The inflammation causes the synovium to thicken and swell.
Over time, this chronic inflammation creates a destructive tissue called pannus. The pannus invades and erodes the surrounding structures. It damages the articular cartilage, which is the smooth, protective layer covering the ends of the bones. It also weakens the ligaments and tendons that stabilize the joint. This process can severely limit the shoulder’s range of motion and strength.
Recognizing the Symptoms of Shoulder RA
Identifying the symptoms of rheumatoid arthritis in the shoulder can sometimes be challenging. The pain may mimic other common shoulder problems but is typically the worst first thing in the morning or with prolonged immobilization. However, RA-related shoulder pain often presents with distinct characteristics. Recognizing these signs early can be helpful for a timely diagnosis and treatment plan.
The most common symptom is pain. This pain is often described as a deep, aching sensation within the joint that typically worsens with movement. A key feature of RA is that it can be symmetrical. If RA affects one shoulder, it may affect the other shoulder as well. This bilateral involvement may suggest an autoimmune condition rather than a mechanical injury.
Stiffness is another hallmark symptom. Patients frequently experience significant stiffness, especially after periods of rest. This is often most pronounced in the morning.
Other common symptoms include:
Swelling and Warmth: The shoulder joint may feel warm to the touch. You might notice visible swelling around the joint capsule.
Limited Range of Motion: As the disease progresses, the shoulder’s ability to move freely decreases. Simple tasks like reaching overhead, dressing, or washing your hair may become difficult.
Crepitus: You may hear or feel a grinding, clicking, or popping sensation when you move your shoulder. This sound, known as crepitus, occurs when the damaged cartilage surfaces rub against each other.
Fatigue and Systemic Symptoms: Since RA is a systemic disease, it affects the entire body. Patients frequently report generalized fatigue, low-grade fever, and a general feeling of being unwell.
The Progression of Rheumatoid Shoulder Disease
Rheumatoid arthritis is a progressive condition. Without effective treatment, the damage to the shoulder joint may worsen over time. One potential consequence is the weakening and tearing of the rotator cuff. The inflammatory pannus tissue can invade the rotator cuff tendons and weaken the tendons’ structure.
When the rotator cuff tears, the head of the humerus is no longer held securely in the center of the glenoid socket. The humeral head may begin to move upward. The bone can then start to rub against the acromion (the top part of the shoulder blade).
This combination of RA-related joint destruction and an irreparable rotator cuff tear is known as rotator cuff arthropathy. This condition can cause severe pain and an inability to lift the arm. At this stage, the joint damage is extensive and many non-surgical treatments may become less effective.
Diagnosis: Finding the Root Cause of Shoulder Pain
Diagnosing rheumatoid arthritis in the shoulder requires a careful and comprehensive evaluation. Your doctor may combine several diagnostic tools to confirm the condition.
The process generally begins with a thorough physical examination and medical history. Your doctor may inquire about the onset, duration, and pattern of your pain and stiffness. They may also assess your range of motion and strength and look for signs of swelling, warmth, and tenderness in the joint.
Blood tests can help confirm a diagnosis of RA. Key markers include:
Rheumatoid Factor (RF): An antibody found in the blood of many people with RA.
Anti-cyclic citrullinated peptide (anti-CCP) antibodies: Their presence can help support the diagnosis even in early stages.
Erythrocyte Sedimentation Rate (ESR) and C-Reactive Protein (CRP): These are general markers of inflammation in the body. Elevated levels may suggest an active inflammatory process.
Imaging studies provide a visual assessment of the joint damage. X-rays are typically the first imaging test performed. They can reveal joint space narrowing, bone erosion, and superior migration of the humeral head. In the early stages, X-rays may appear normal.
A magnetic resonance imaging (MRI) scan can show inflammation of the synovium (synovitis). It can also visualize the condition of the soft tissues, including the rotator cuff tendons. An MRI is often necessary to determine if a rotator cuff tear has occurred.
Treatment Options: A Comprehensive Approach to Shoulder RA
Treatment for rheumatoid arthritis aims to reduce inflammation, control pain, slow disease progression, and maintain joint function. Treatment plans are highly individualized and typically involve a combination of medical management and physical therapy. In advanced cases, surgical intervention may be recommended.
Non-Surgical Management
Medical therapy’s goal is to suppress the overactive immune system.
Disease-Modifying Anti-Rheumatic Drugs (DMARDs): These medications may help slow the progression of RA.
Biologic Agents: These are a newer class of DMARDs. They target specific parts of the immune system and may reduce inflammation and prevent joint damage.
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): These drugs help manage pain and reduce inflammation.
Corticosteroids: A corticosteroid injection may provide temporary but significant pain relief.
Physical therapy plays a key role in maintaining function. A physical therapist designs a program to help maintain range of motion, strengthen muscles, and reduce pain.
Surgical Intervention
When non-surgical treatments fail to control pain or when joint destruction is severe, surgery may become the recommended option. An expert shoulder specialist can determine the most appropriate procedure based on the extent of the damage.
In the early stages, a minimally invasive procedure called arthroscopy may be performed. The surgeon can use small instruments to clean out the inflamed synovium. This procedure, called a synovectomy, may help reduce pain and slow the disease progression.
Shoulder joint replacement involves replacing the damaged joint surfaces with artificial components. There are two main types of shoulder replacement used for RA:
Total Shoulder Arthroplasty: This procedure replaces both the ball (humeral head) and the socket (glenoid) with prosthetic parts. It is typically used when the rotator cuff is intact or repairable.
Reverse Total Shoulder Arthroplasty: This innovative procedure is frequently recommended for patients with rotator cuff arthropathy. The “ball” and “socket” components are reversed. The ball is placed on the shoulder blade, and the socket is placed on the arm bone. This design allows the deltoid muscle, rather than the damaged rotator cuff, to power the arm. For many patients, reverse shoulder replacement has provided excellent pain relief and restored the ability to lift the arm, even in the presence of a massive rotator cuff tear.
Summary
The answer to the question, “Can you get rheumatoid arthritis in your shoulder?” is a resounding yes. This autoimmune condition can cause pain and disability in the shoulder joint. It attacks the joint lining, frequently leading to progressive damage to cartilage, bone, and the rotator cuff tendons. If you are experiencing persistent shoulder pain, stiffness, or loss of motion, especially if it affects both sides, seeking a consultation with a shoulder specialist can be a first step toward regaining control of your health and mobility.
Frequently Asked Questions
Is shoulder pain from RA different from pain caused by osteoarthritis?
Often, yes. Osteoarthritis (OA) is a “wear-and-tear” condition. OA pain typically worsens with activity and improves with rest. RA pain is inflammatory. It is frequently worse after rest, particularly in the morning, with stiffness lasting for hours. RA also tends to affect both shoulders symmetrically, which is less common with OA.
Does RA always lead to a rotator cuff tear in the shoulder?
Not always, but it can increase the risk. The chronic inflammation from RA weakens the tendons and may make them more susceptible to tearing.
Is the AC joint also affected by rheumatoid arthritis?
Yes, the acromioclavicular (AC) joint contains synovial lining and can be affected by RA. Inflammation in the AC joint typically causes pain at the top of the shoulder. Treatment for AC joint RA is usually non-surgical, involving injections and anti-inflammatory medication.



