As a shoulder specialist, I’ve seen how a shoulder injury can quietly erode the activities patients care about most, such as throwing a baseball, playing tennis or pickleball, swimming laps, or simply sleeping through the night without waking up in pain. One injury that often catches people off guard is a SLAP tear of the shoulder. SLAP tears of the shoulder are commonly misunderstood, partly because the symptoms can mimic so many other shoulder conditions. Understanding the anatomy, how these tears develop, and what your treatment options may look like is a meaningful first step toward getting the right care.
Key Takeaways
- SLAP stands for Superior Labrum Anterior to Posterior. It describes a tear in a specific part of the fibrocartilage ring of the glenoid that helps stabilize the shoulder’s ball-and-socket joint.
- Common symptoms may include deep shoulder pain, a clicking or catching sensation, and discomfort during overhead or throwing activities.
- Treatment depends heavily on the type and severity of the tear, your age, activity level, and how the shoulder responds to conservative care. Not every SLAP tear requires surgery.
- I have published on this specific topic in the peer-reviewed medical literature, and this provides additional details on this topic.
What Is a SLAP Tear?
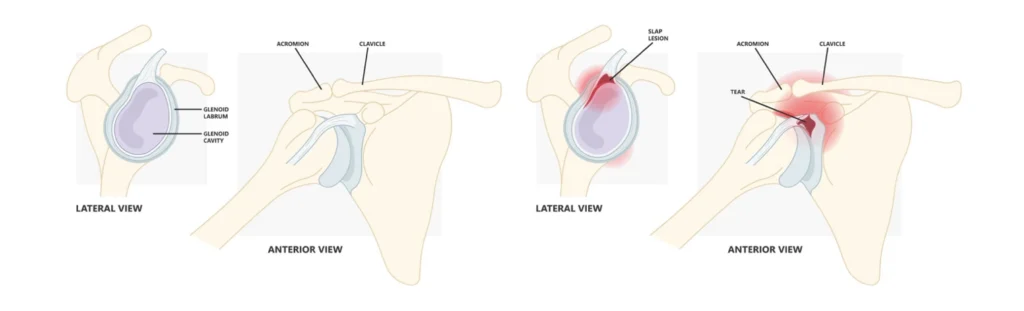
To understand a SLAP tear, it helps to first understand how the shoulder is built. Your shoulder is a ball-and-socket joint. The ball is the rounded top of your upper arm bone, called the humerus. The socket is a shallow, cup-shaped surface on your shoulder blade called the glenoid. Because that socket is naturally quite shallow, a ring of fibrocartilage called the labrum lines its rim to add depth and help keep the ball from slipping out of place.
The labrum does more than deepen the socket, though. It also serves as an attachment point for the long head of the biceps tendon, which anchors directly into the top of the labrum. SLAP stands for Superior Labrum Anterior to Posterior. A SLAP tear is a specific injury to the top portion of the labrum, running from the front (anterior) to the back (posterior) of the biceps anchor.
When this area tears, the stability of the shoulder can be affected, particularly during overhead movements and rotational activities. The shoulder may not feel right, and for overhead athletes especially, even a partial tear can have a meaningful impact on performance and comfort.
What Causes SLAP Tears?
SLAP tears can develop in a few different ways, and the mechanism of injury often gives me useful clues during evaluation.
Acute injuries are one common cause. A fall onto an outstretched hand, a forceful traction injury to the arm, such as catching yourself mid-fall or being yanked suddenly, or a direct blow to the shoulder can all cause the labrum to tear at the top of the socket. Shoulder dislocations can also damage the labrum, including the superior portion.
Repetitive overhead activity is another potential cause. Baseball pitchers, swimmers, volleyball players, and tennis players repeatedly stress the top of the labrum through throwing or swinging motions. Over time, that cumulative load can cause the labrum and biceps anchor to gradually fray and eventually tear. Age-related degeneration also plays a role. As we get older, the labrum loses elasticity and resilience.
Certain individuals may face a higher risk, including:
- Overhead athletes, particularly baseball pitchers and throwers
- Swimmers and tennis or volleyball players who repeatedly stress the shoulder
- Workers who perform repetitive lifting or overhead tasks
- Anyone who has experienced a shoulder dislocation or significant fall
- Older adults with naturally occurring degenerative changes in the shoulder
Types of SLAP Tears
Not all SLAP tears are created equal, and the type of tear present matters considerably when it comes to choosing the right treatment. Surgeons commonly use a classification system, such as the Snyder classification, to describe the extent and pattern of the injury. The four most clinically relevant types are:
Type I: The top of the labrum shows fraying and degeneration but remains attached to the socket rim. This type is commonly associated with normal aging and may not always produce significant symptoms.
Type II: The superior labrum and the biceps tendon anchor lift away from the glenoid, creating instability at that attachment point. Type II tears tend to be more symptomatic and may require treatment.
Type III: A bucket-handle tear of the superior labrum where a flap of tissue tears but the biceps anchor remains intact. The torn fragment can occasionally flip into the joint and cause mechanical symptoms like locking or catching.
Type IV: Similar to Type III, but the tear extends into the biceps tendon itself. These injuries tend to be more complex and may involve additional considerations during treatment planning.
Recognizing the Symptoms
One of the things that makes SLAP tears of the shoulder particularly challenging is that symptoms can closely resemble other shoulder conditions. Symptoms alone rarely tell the whole story, which is why thorough evaluation matters so much.
That said, certain patterns come up consistently. Deep shoulder pain is a frequent complaint. Patients frequently describe it as being “inside” the joint rather than at the surface. Pain tends to worsen with overhead activity, reaching across the body, throwing, or any motion that loads the biceps anchor. Some patients describe a clicking, popping, or catching sensation with certain shoulder movements.
Individuals may notice decreased strength with pushing, pulling, or carrying. Others describe a vague sense that the shoulder feels “off” or unstable. In overhead athletes, a loss of throwing velocity or accuracy, sometimes before pain becomes prominent, can be an early sign worth evaluating.
Getting a Diagnosis
Diagnosing a SLAP tear starts with a detailed conversation. I want to understand exactly how the injury happened, when symptoms began, and what activities make them better or worse. A physical examination will follow.
Following the initial conversation and physical exam, imaging tests may be ordered. X-rays don’t show soft tissue injuries directly, but they help rule out other issues like fractures or arthritis. An MRI may be used to visualize the soft tissues. MRI is not always accurate in diagnosing SLAP tears, however the accuracy can be improved with injecting a contrast agent into the shoulder prior to the MRI. This is called an ‘MRI-arthrogram’. However, false-positives may continue and therefore it is the clinical examination which is most important in the hands of a shoulder specialist such as myself.
Treatment Options: A Highly Individual Decision
The right treatment plan depends on the type and severity of the tear, your age and overall health, your activity demands, and how your shoulder has responded to prior treatment, if any.
Non-Surgical Treatment
For many patients, non-surgical management is a reasonable and often effective first approach. It may involve a structured physical therapy program focused on strengthening the muscles around the shoulder, improving joint stability, and correcting movement patterns that place excessive stress on the labrum. Anti-inflammatory medications may help manage pain during the recovery process, and activity modification reduces load on the shoulder while symptoms improve. In some cases, a corticosteroid injection may be considered to help control inflammation enough to allow full participation in therapy.
Many patients experience symptom improvement through a well-structured conservative program. In overhead athletes, however, non-surgical treatment can be more limited in its effectiveness, particularly when the biceps anchor is destabilized and a return to competitive throwing is the goal.
Surgical Treatment
When conservative treatment hasn’t provided adequate relief, when the tear is more complex, or when a patient needs to return to overhead sports or demanding physical work, surgery may be considered as a next step. The most common approach is shoulder arthroscopy, a minimally invasive technique where a small camera and instruments are inserted through tiny incisions to visualize and address the tear directly.
Depending on the condition, different repairs may be performed. In a SLAP repair, suture anchors are used to reattach the torn labrum and biceps anchor to the rim of the socket. Biceps tenodesisdetaches the long head of the biceps tendon from the torn labral anchor and reattaches it lower on the humerus, with the goal of relieving tension on the damaged area. SLAP repair today is less commonly performed than biceps tenodesis as the recovery time is faster and often times there is additional pathology involving the long head biceps tendon as well that can be addressed better with tenodesis.
Summary
SLAP tears of the shoulder involve a specific injury to the top of the labrum and its biceps tendon attachment, structures that contribute meaningfully to shoulder stability, particularly during overhead and rotational movement. Diagnosis requires careful history-taking, a targeted physical examination, and imaging. Treatment ranges from structured physical therapy and activity modification to arthroscopic SLAP repair or biceps tenodesis, depending on the tear type and each patient’s individual goals. Working with an expert shoulder specialist to develop a personalized plan may help support your treatment and recovery.
Frequently Asked Questions
What does a SLAP tear feel like?
SLAP tears of the shoulder often produce a deep, aching pain inside the joint. Pain tends to worsen with overhead activity, throwing, or movements that load the biceps. Many patients also describe a clicking, popping, or catching sensation during certain shoulder movements. Symptoms vary considerably from person to person, which is why an evaluation is more reliable than relying on symptoms alone.
Can a SLAP tear heal without surgery?
Some SLAP tears, particularly less severe or degenerative tears, may respond well to non-surgical treatment, including physical therapy and activity modification. Other tears may be less likely to fully resolve with conservative care. Whether surgery is appropriate depends on a number of factors specific to your injury, your activity goals, and how your shoulder responds to treatment over time.
Will I be able to return to throwing sports after treatment?
Many overhead athletes do return to throwing after SLAP repair surgery or biceps tenodesis, though the timeline and level of return depend on several factors, such as the type and extent of the tear, the surgical approach used, and the quality of rehabilitation. Return to competitive throwing is a gradual process that typically follows a structured interval program. Discussing realistic expectations for your specific situation early on is an important part of planning your care.



