Rotator cuff injuries are a common cause of shoulder pain and disability, affecting millions of individuals annually. When conservative treatments fail to alleviate symptoms or restore function, rotator cuff surgery may become the recommended treatment option. In this post, we’ll take a close look at rotator cuff surgery, exploring the procedure, preparation, and recovery process.
Key Takeaways
- Rotator cuff surgery is a procedure to repair torn tendons in the shoulder, frequently performed when non-surgical treatments are ineffective or for severe tears. For some traumatic, full-thickness tears in active patients, a more immediate surgical approach is recommended.
- Types of surgeryinclude arthroscopic (minimally invasive, most common) and open repairs, sometimes chosen based on tear size and complexity.
- Pre-operative preparation involves a thorough medical evaluation, medication review, and understanding the procedure and recovery plan.
- Post-operative recovery is a multi-stage process involving immobilization, pain management, and a structured physical therapy program.
The Rotator Cuff: Anatomy and Function
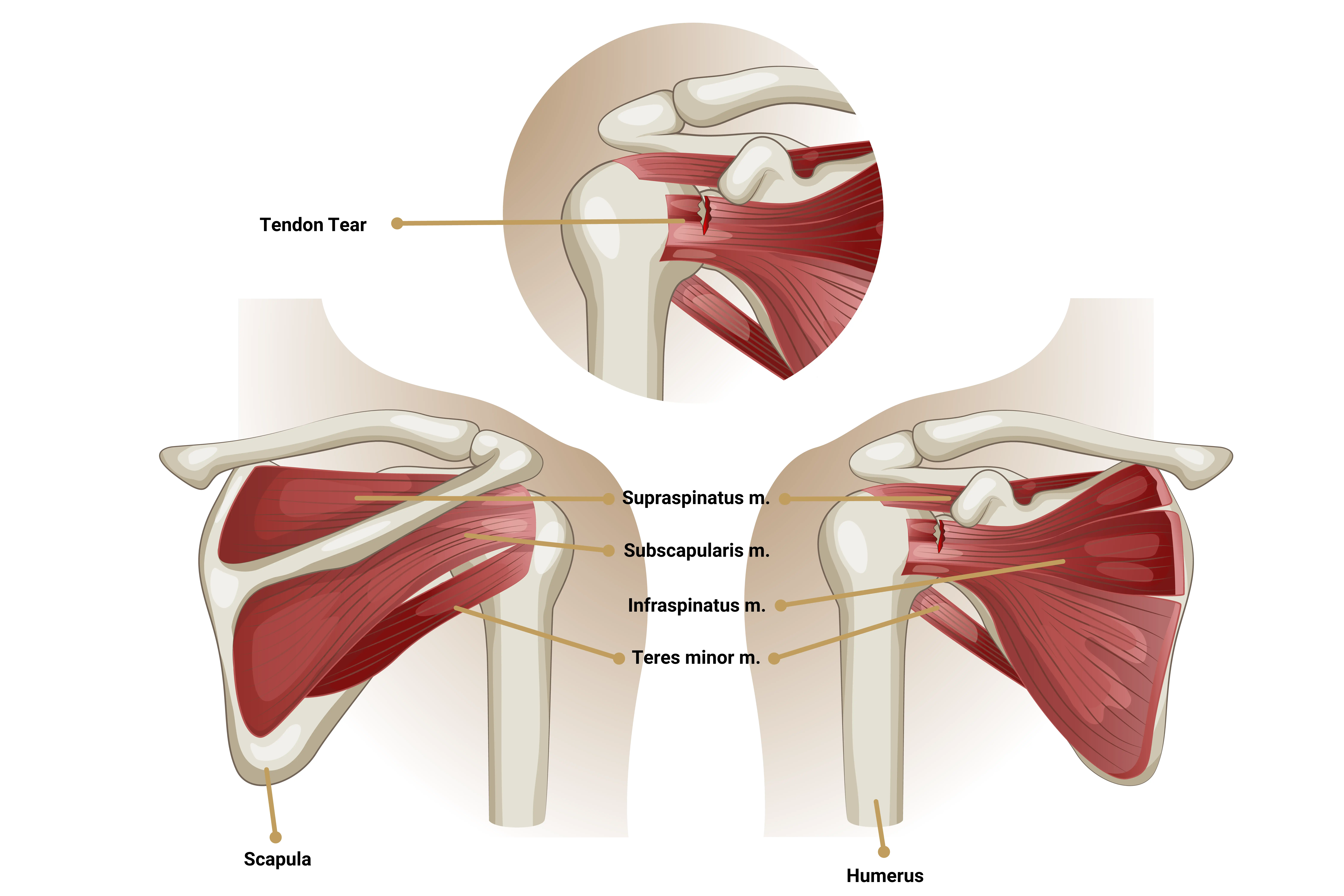
The rotator cuff is a group of four muscles and their tendons that surround the shoulder joint. Providing stability and enabling a wide range of motion. These muscles, the supraspinatus, infraspinatus, teres minor, and subscapularis, work in concert to lift and rotate the arm. The shoulder joint itself is a ball-and-socket joint, where the head of the humerus (upper arm bone) fits into a shallow socket in the shoulder blade (scapula), known as the glenoid. The rotator cuff tendons essentially form a cuff around the humeral head, holding it firmly in the glenoid socket.

This intricate arrangement allows for complex movements such as lifting, reaching, and rotating the arm. Making the shoulder one of the most mobile joints in the human body. When these tendons are injured or torn, the stability and function of the shoulder can be severely compromised, leading to pain, weakness, and limited range of motion.
Causes and Diagnosis of Rotator Cuff Tears
Rotator cuff tears can result from a variety of factors, broadly categorized into acute injuries and degenerative tears. Acute tears may occur due to a sudden event. These can include falling on an outstretched arm, lifting a heavy object with a jerking motion, or a direct blow to the shoulder. These are common in athletes involved in overhead sports like baseball, tennis, or swimming, as well as in individuals whose occupations require repetitive overhead activities.
Degenerative tears, on the other hand, develop gradually over time. They are more common in older adults and are often attributed to several contributing factors including repetitive stress, lack of blood supply, and bone spurs.
Diagnosing a Rotator Cuff Tear
Accurate diagnosis guides effective treatment. Your doctor will typically begin with a thorough physical examination, assessing the shoulder for tenderness, range of motion, and strength. Specific tests designed to evaluate the integrity of each rotator cuff tendon may be performed. Imaging studies are commonly used to confirm the diagnosis and determine the extent of the tear:
- X-rays: X-rays can help identify bone spurs, arthritis, or other bone-related issues that may contribute to shoulder pain.
- Magnetic Resonance Imaging (MRI): An MRI provides detailed images of soft tissues, allowing the physician to visualize the tear, its size, and its location.
- Ultrasound: Ultrasound can also be used to detect rotator cuff tears and assess the condition of the tendons, offering a dynamic view of the shoulder in motion.
- CT Scan: Sometimes a CT scan is used, with or without injection of a contrast agent into the joint prior to the scan, if an MRI is not feasible because of existing hardware in the shoulder joint.
Non-Surgical Treatment Options
Before considering surgery, many patients with rotator cuff tears will undergo a course of non-surgical treatment. These approaches aim to reduce pain and improve function. Non-surgical options can be effective for partial tears, smaller tears, degenerative tears, or in patients who are less active or have health risks that make surgery less advisable. Common non-surgical treatments include:
- Rest and Activity Modification: Avoiding activities that exacerbate shoulder pain is often the first step. This might involve temporary cessation of sports or occupational tasks that require overhead arm movements.
- Pain Management: Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) can help reduce pain and inflammation.
- Physical Therapy: A structured physical therapy program is frequently a cornerstone of non-surgical treatment. A physical therapist will guide patients through exercises designed to restore range of motion, strengthen the shoulder and surrounding muscles, and improve overall shoulder mechanics.
- Injections: Corticosteroid injections into the shoulder joint may provide temporary pain relief and reduce inflammation. Newer ‘biologic’ agents such as platelet-rich-plasma (PRP), peptides, or stem-cells have not shown consistent results and may not be covered by insurance, yet but may be considered.
If these conservative measures do not provide adequate relief after several months, or if the tear is large or significantly impacts daily activities, surgical intervention may be considered. The decision to proceed with rotator cuff surgery is a collaborative one between the patient and an experienced orthopedic surgeon.
Types of Rotator Cuff Surgery
Advances in surgical techniques have led to less invasive and more effective ways to repair rotator cuff tears. The primary goal of all surgical approaches is to repair or reattach the torn tendon back to its original site on the head of the humerus (upper arm bone). The choice of surgical method depends on factors such as the size and complexity of the tear, the patient’s anatomy, and the surgeon’s experience.
Arthroscopic Repair (Minimally Invasive)
This is currently the most common method for repairing rotator cuff tears. During an arthroscopic procedure, the surgeon makes several small incisions around the shoulder joint. A small camera, called an arthroscope, is inserted through one incision, displaying a live video feed of the shoulder’s interior on a monitor. Miniature surgical instruments are then inserted through other small incisions to perform the repair.
Advantages of Arthroscopic Repair:
- Minimally Invasive: Smaller incisions result in less soft tissue disruption, potentially leading to less pain and a quicker initial recovery.
- Enhanced Visualization: The arthroscope provides a magnified view of the shoulder joint, allowing the surgeon to thoroughly assess the tear and address other concurrent issues like arthritis, bone spurs, or biceps tendon problems.
- Outpatient Procedure: Most arthroscopic repairs are performed on an outpatient basis, meaning the patient can go home the same day.
Open Repair
In an open repair, the surgeon makes a larger incision over the shoulder. The surgeon directly visualizes the shoulder structures and performs the repair.
Advantages of Open Repair:
- Suitable for Complex Tears: Often preferred for very large or complex tears, or when additional reconstruction (e.g., tendon transfer) is required.
- Direct Access: Allows for a direct, unobstructed view of the entire surgical field.
Historically, open repair was the first technique used. While modern techniques have largely shifted towards arthroscopic methods, open repair remains an option for specific cases.
Preparing for Rotator Cuff Surgery
Proper preparation for rotator cuff surgery can be essential for optimizing outcomes and ensuring a smooth recovery. Your healthcare team will provide detailed instructions, but generally, preparation involves several key steps.
Medical Evaluation and Pre-operative Testing
Before surgery, your medical team will conduct a thorough evaluation to ensure you are in good health and ready for the procedure. It is important to provide your doctor with a complete list of all medications, supplements, and herbal remedies you are currently taking. Certain medications may need to be discontinued days or weeks before the operation, usually those that can cause increased bleeding such as NSAIDs. Your surgeon will offer specific instructions tailored to your situation.
Practical Preparations
Practical arrangements can make the recovery period smoother and less stressful. Plan for someone to drive you home after the procedure and assist with daily tasks such as cooking, cleaning, and personal care during the first few days or weeks when your arm will be immobilized. Preparing your home in advance is also important. Place frequently used items within easy reach, set up a comfortable recovery space, and remove any tripping hazards to prevent falls.
Wearing loose, easy-to-remove clothing can make dressing much easier while your mobility is limited. In some cases, your surgeon may recommend meeting with a physical therapist before surgery to review your post-operative rehabilitation plan and learn key exercises in advance. Finally, be sure to fully understand the procedure, potential risks, and recovery expectations. Ask any questions you may have and carefully review the consent form before signing.
Post-Operative Recovery and Rehabilitation
The journey to full recovery after rotator cuff surgery is a gradual process that requires patience, commitment, and strict adherence to your surgeon’s and physical therapist’s instructions. While timelines may vary per patient, the recovery period typically spans several months, with different stages focusing on protection, regaining motion, and building strength.
Immediate Post-Operative Period
- Pain Management: You may experience pain after surgery, which is a common part of the healing process. It is important to use prescribed medications as directed. Ice packs applied to the shoulder may also help reduce swelling and pain.
- Immobilization: Your arm may be kept in a sling or immobilizer for several weeks to protect the healing tendon. The duration depends on the size and type of tear, as well as the quality of your tissue.
- Wound Care: Keep the surgical incision clean and dry. Your surgeon will provide specific instructions on wound care.
- Passive Range of Motion (PROM): Within the first few weeks, your physical therapist will typically begin passive exercises. During PROM, the therapist moves your arm and shoulder through various ranges of motion without you actively engaging your shoulder muscles. This helps prevent stiffness and scar tissue formation while protecting the repair.
Early Rehabilitation
- Active-Assisted and Active Range of Motion (AAROM/AROM): As the tendon begins to heal, you may gradually progress to active-assisted exercises, where you use your other arm or a pulley system to help move the operated arm. Eventually, you may start active range of motion exercises, moving your shoulder independently within prescribed limits.
- Gentle Strengthening: Your physical therapist may introduce gentle isometric exercises and light strengthening activities for the shoulder and surrounding muscles. The focus remains on protecting the healing tendon while gradually building strength.
Intermediate to Advanced Rehabilitation
- Progressive Strengthening: This phase focuses on progressive strengthening exercises tailored to your individual needs and activity goals. This includes resistance exercises using bands, light weights, and bodyweight exercises to rebuild muscle strength and endurance.
- Functional Training: Exercises may become more functional, mimicking activities of daily living, work-related tasks, or sport-specific movements. The goal is to restore full strength, coordination, and proprioception (awareness of joint position).
- Return to Activities: Your surgeon and physical therapist will guide your gradual return to full activities, including sports or heavy lifting. This is a carefully monitored process to prevent re-injury.
Full recovery generally takes anywhere from 4 to 6 months, or up to a year for more complex cases.
Summary
Rotator cuff surgery can be a recommended treatment option for individuals suffering from persistent pain and functional limitations due to rotator cuff tears. While non-surgical approaches can be explored initially, surgery provides a solution for many for a more durable result. Full-thickness rotator cuff tears that are ignored for a long time will degenerate and eventually become irreparable. By being well-informed and actively participating in their care, patients can help improve their chances of a successful outcome, leading to reduced pain, restored shoulder function, and an improved quality of life.
Frequently Asked Questions
How long will I be in a sling after surgery?
The duration of sling immobilization varies but is typically between 4 to 6 weeks. This period is important for protecting the healing tendon. Your surgeon will provide specific instructions based on the nature of your tear and the repair performed.
When can I return to work after rotator cuff surgery?
The timeline for returning to work depends heavily on the nature of your job. For sedentary jobs, you might be able to return within a few weeks, often with restrictions on using the operated arm. For jobs requiring manual labor, lifting, or overhead activities, it could take several months. Your surgeon and physical therapist will guide you on a safe return to work.
Is physical therapy mandatory after rotator cuff surgery?
Yes, physical therapy is often an essential part of a successful recovery. It supports regaining strength, flexibility, and full range of motion. Skipping or not fully committing to physical therapy may increase the risk of suboptimal outcomes.



