The shoulder represents one of the most complex and mobile joints in the human body. This remarkable range of motion, while beneficial for daily activities, can also make the shoulder vulnerable to various injuries and conditions. Understanding the most common shoulder problems can help you recognize symptoms early and seek appropriate treatment when needed.
Key Takeaways
- Shoulder pain can result from various conditions, ranging from rotator cuff tears to arthritis.
- Early recognition of symptoms may allow for earlier evaluation and management, which can help reduce the risk of progression in some cases.
- Most shoulder conditions respond well to conservative treatments, though some may require surgical intervention.
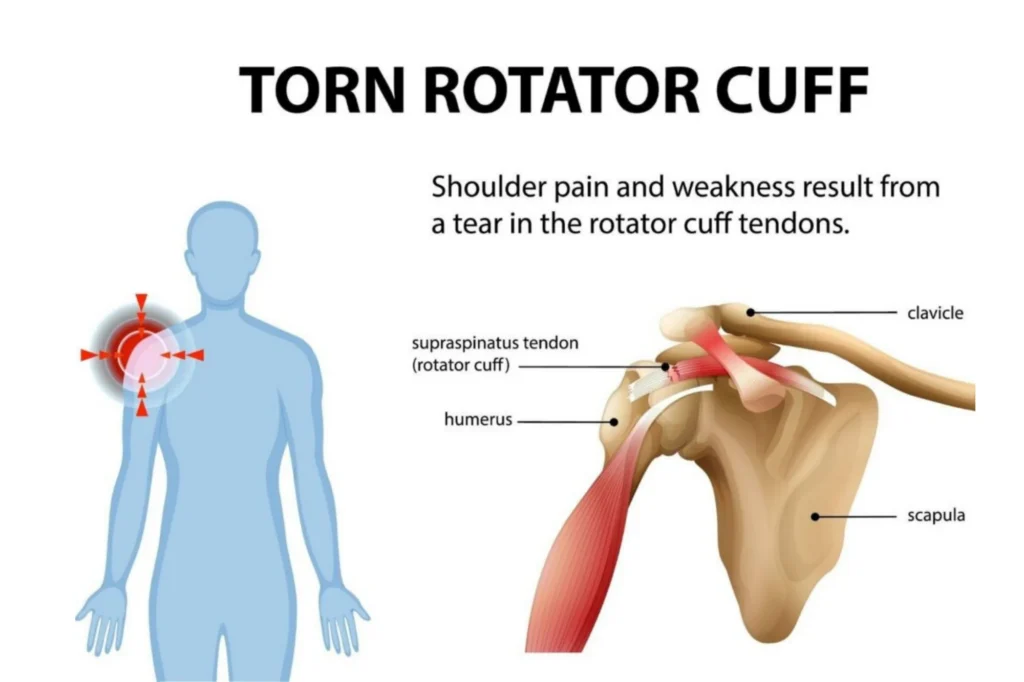
Rotator Cuff Tears
The rotator cuff consists of four muscles and their tendons that surround the shoulder joint. These structures work together to provide stability and enable arm movement. Rotator cuff tears represent one of the most common shoulder problems, affecting people of all ages, though they tend to occur more frequently in individuals over 40.
Causes
Rotator cuff tears can develop through two primary mechanisms. Acute tears often result from sudden injury, such as lifting heavy objects, falling on an outstretched arm, or experiencing sports trauma. Degenerative tears develop gradually over time due to repetitive stress, aging, or reduced blood supply to the tendons.
Symptoms
People with rotator cuff tears often experience pain, particularly when lifting objects or reaching overhead. The discomfort may worsen at night, making it difficult to sleep on the affected shoulder. Weakness in the shoulder and arm can develop, making routine activities like combing hair or reaching for items on high shelves challenging.
Some individuals report a crackling sensation when moving the shoulder in certain positions. The severity of symptoms can vary considerably depending on the size and location of the tear. Small tears might produce minimal symptoms initially, while complete tears typically cause more pronounced pain and functional limitations.
Treatment Options
Conservative management may prove effective for many rotator cuff tears, particularly smaller ones. Rest, ice application, and anti-inflammatory medications can help reduce pain and swelling. Physical therapy commonly plays a role in strengthening the surrounding muscles and improving shoulder function.
When conservative approaches don’t provide adequate relief, surgical intervention might become necessary. Arthroscopic repair techniques allow many rotator cuff tears to be addressed using minimally invasive approaches with small incisions.
Shoulder Impingement Syndrome
Shoulder impingement occurs when the rotator cuff tendons become compressed between the bones of the shoulder joint. The space between the acromion and rotator cuff is relatively narrow. If inflammation, bone spurs, or tissue thickening reduce this space, the tendons may become irritated during overhead movements.
Athletes who perform repetitive overhead motions, such as swimmers and baseball pitchers, may be particularly susceptible. However, the condition can also develop in individuals whose work requires frequent overhead reaching.

Recognizing Symptoms
Pain during overhead activities is a common symptom of shoulder impingement. The discomfort often develops gradually and may initially appear only during specific movements. As the condition progresses, pain might occur even during rest, especially at night. Weakness and difficulty raising the arm above shoulder level can develop over time. Some people describe a catching or clicking sensation when moving the shoulder.
Treatment Approaches
Initial treatment for shoulder impingement usually focuses on reducing inflammation and modifying activities that aggravate symptoms. Physical therapy emphasizes strengthening the rotator cuff muscles and improving posture to create more space in the shoulder joint.
Corticosteroid injections may provide temporary relief when other conservative measures prove insufficient. Surgery might be considered if symptoms persist despite several months of conservative treatment. Arthroscopic procedures may be used to remove bone spurs and inflamed tissue, potentially creating more space for the rotator cuff tendons.
Frozen Shoulder (Adhesive Capsulitis)
Frozen shoulder develops when the shoulder capsule, the connective tissue surrounding the joint, becomes thick and tight. This condition typically progresses through distinct stages and can significantly limit shoulder mobility.
The exact cause of frozen shoulder remains somewhat unclear, though certain factors appear to increase susceptibility. People with diabetes or thyroid disorders may face a higher risk. Prolonged shoulder immobilization following injury or surgery can also trigger the condition.
Women between 40 and 60 years old appear to develop frozen shoulder more frequently. Previous shoulder injuries may predispose individuals to this condition, though it can also occur without any obvious precipitating event.
Progression and Symptoms
Frozen shoulder typically progresses through three stages: increasing pain and stiffness (freezing), persistent stiffness with limited motion (frozen), and gradual return of mobility (thawing), often over many months. Pain intensity may vary throughout the day and often worsens with attempted movement. Simple activities like reaching behind the back or putting on a coat can become extremely difficult or impossible during the frozen stage.
Management Strategies
Conservative treatment remains the primary approach for frozen shoulder, as many cases gradually improve over time, although recovery may take many months and varies by individual. Physical therapy focusing on gentle stretching exercises can help maintain as much mobility as possible.
Anti-inflammatory medications and corticosteroid injections may help manage pain, particularly during the freezing stage. For cases where conservative treatment doesn’t provide adequate improvement, surgical options such as manipulation under anesthesia or arthroscopic capsular release might be considered.
Shoulder Arthritis
Arthritis affecting the shoulder can significantly impact quality of life and daily function. While less common than hip or knee arthritis, shoulder arthritis can cause substantial discomfort and disability.
Types and Causes
Osteoarthritis, the wear-and-tear form of arthritis, develops when cartilage cushioning the shoulder joint gradually deteriorates. This type typically affects older adults or individuals with a history of shoulder injuries. Rheumatoid arthritis, an autoimmune condition, can also affect the shoulder joint. Post-traumatic arthritis may develop following significant shoulder injuries, such as fractures or dislocations. The inflammatory response and structural changes from these injuries can accelerate cartilage breakdown.
Symptoms and Functional Impact
Pain that worsens with activity represents the primary symptom of shoulder arthritis. The discomfort may be accompanied by stiffness, particularly after periods of inactivity. Individuals may notice grinding, clicking, or popping sensations during shoulder movement. As arthritis progresses, stiffness, weakness, and night pain may develop, making daily activities more difficult.
Treatment Spectrum
Early-stage shoulder arthritis often responds well to conservative measures. Activity modification, physical therapy, and anti-inflammatory medications can help manage symptoms. Corticosteroid injections may provide temporary relief for moderate to severe pain.
When conservative treatments no longer provide adequate symptom control, surgical options may need consideration. Shoulder replacement surgery, including both total shoulder replacement and reverse shoulder replacement, has advanced considerably in recent years. These procedures are designed to reduce pain and improve function for appropriately selected candidates.
Shoulder Instability and Dislocations
Shoulder instability occurs when the structures that normally keep the upper arm bone centered in the shoulder socket become damaged or loose. This condition can range from subtle subluxation (partial dislocation) to complete dislocation.
Traumatic injuries, particularly those involving forceful impact or falling on an outstretched arm, commonly cause shoulder dislocations. Athletes participating in contact sports or activities involving overhead motions may face increased risk. Once a shoulder dislocates, the supporting structures sustain damage that may predispose the joint to future instability.
Some individuals have naturally loose ligaments, while repetitive overhead activity can gradually stretch supporting structures and contribute to instability.
Signs of Instability
People with shoulder instability often describe a feeling that their shoulder is slipping or about to pop out of place. Visible deformity occurs with complete dislocations, typically accompanied by severe pain and inability to move the arm. Recurrent partial dislocations may cause intermittent pain, weakness, and apprehension when moving the arm into certain positions. Numbness or tingling in the arm may occur if nearby nerves are irritated or affected during a dislocation. After the shoulder returns to its normal position, pain and swelling typically persist for several days or weeks.
Treatment Considerations
First-time dislocations usually require reduction, a procedure where the shoulder is carefully manipulated back into its proper position. Following reduction, a period of immobilization and physical therapy helps restore strength and stability. However, the risk of recurrent dislocations remains elevated, particularly in younger, active individuals.
Surgical intervention may be recommended for recurrent instability or when significant structural damage has occurred. Arthroscopic procedures can repair torn ligaments and tighten loose capsular tissue. Open surgical techniques might be necessary for more complex cases involving bone loss or failed previous surgeries.
Shoulder Bursitis and Tendinitis
Bursitis and tendinitis represent inflammatory conditions that frequently affect the shoulder. While distinct problems, they often occur together and produce similar symptoms.
Bursae are fluid-filled sacs that cushion bones and soft tissues, most commonly the subacromial bursa in the shoulder.
Tendinitis involves inflammation of the tendons, most commonly affecting the biceps tendon or rotator cuff tendons. Repetitive overhead activities, aging, and sudden increases in activity level can all contribute to tendon inflammation.
Symptom Patterns
Sharp or aching pain during movement characterizes both conditions. The discomfort typically worsens with overhead activities and may extend down the arm. Tenderness when touching the affected area can help localize the problem.
Stiffness may develop, particularly after periods of rest. Some individuals notice swelling around the shoulder, though this isn’t always present. Night pain can interfere with sleep, especially when lying on the affected side.
Treatment Protocols
Rest and activity modification form the foundation of treatment for both bursitis and tendinitis. Avoiding activities that aggravate symptoms allows inflammation to subside. Ice application can help reduce pain and swelling, particularly in the acute phase.
Physical therapy emphasizes gentle stretching initially, progressing to strengthening exercises as symptoms improve. Anti-inflammatory medications can help manage discomfort. Corticosteroid injections may be considered for persistent cases. In some cases, surgery may be considered if symptoms persist despite conservative treatment.
Summary
The most common shoulder problems include rotator cuff tears, impingement syndrome, frozen shoulder, arthritis, instability, bursitis, and tendinitis. Early recognition of shoulder symptoms and prompt evaluation by an expert shoulder specialist may guide timely treatment decisions. Many shoulder conditions improve with conservative management, including physical therapy, activity modification, and anti-inflammatory treatments. When these approaches don’t provide adequate relief, advanced surgical techniques may be recommended.
Frequently Asked Questions
How long should I wait before seeing a doctor about shoulder pain?
While minor shoulder discomfort that resolves within a few days might not require immediate medical attention, you should consider scheduling an evaluation if pain persists beyond a week or two, worsens despite rest, or significantly limits your daily activities.
Can shoulder problems heal on their own?
Some shoulder conditions, particularly minor strains or mild bursitis, may improve with rest and self-care measures. However, certain problems such as full-thickness rotator cuff tears or recurrent shoulder instability may not improve without medical evaluation and treatment. Even conditions that might improve spontaneously, such as frozen shoulder, may benefit from professional management.
Will I need surgery for my shoulder problem?
Many shoulder conditions respond well to conservative treatment, including physical therapy, medications, and activity modification. Surgery typically becomes necessary only when conservative measures fail to provide adequate symptom relief or when structural damage requires repair. Your shoulder specialist can help determine whether surgical intervention might benefit your specific situation.



