When most people hear the word “arthritis,” they picture an older adult. However, shoulder arthritis in younger patients is more common than many realize, and it can be just as limiting. I’ve seen it in athletes whose shoulders have endured years of repetitive stress, in young adults dealing with the lasting effects of injuries from their twenties, and in patients with underlying conditions that accelerate joint breakdown well before typical wear-and-tear would set in. If you’re under 50 and have been diagnosed with shoulder arthritis, or you’re starting to notice persistent shoulder pain or stiffness, this post can help you better understand what may be happening and what your options might look like.
Key Takeaways
- Shoulder arthritis in younger patients can develop as a result of prior injury, repetitive overuse, inflammatory conditions, or other underlying causes.
- Symptoms may include persistent shoulder pain, stiffness, grinding sensations, and difficulty performing everyday tasks.
- Not all cases require surgery. Many younger patients respond well to non-surgical treatments, at least initially.
- For patients who do need surgery, there are options designed to preserve as much of the natural joint as possible.
What Is Shoulder Arthritis?
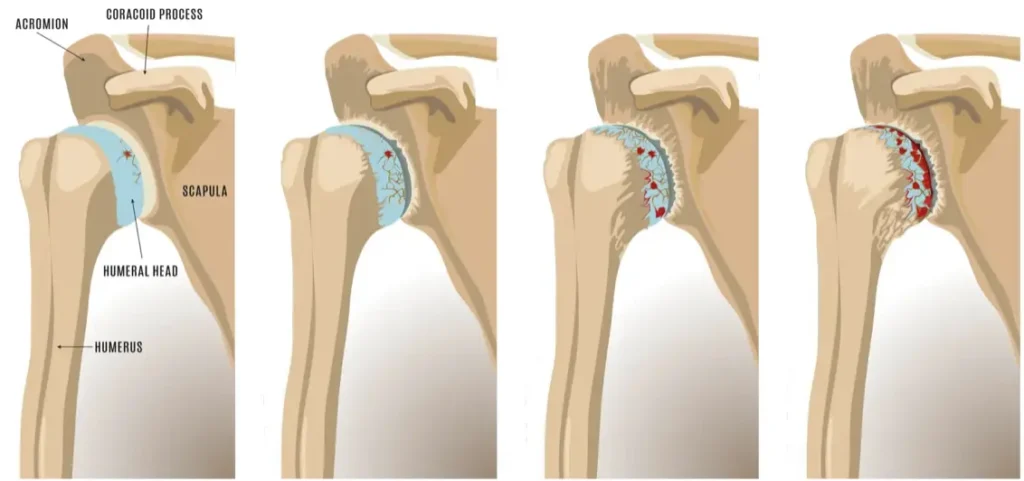
The shoulder is a ball-and-socket joint made up of the humerus (the upper arm bone) and the glenoid (the socket in your shoulder blade). A smooth layer of cartilage covers the surfaces of both the ball and the socket. This cartilage allows the two surfaces to glide against each other with very little friction, making it possible for your shoulder to move fluidly in nearly every direction.
Arthritis develops when the cartilage breaks down. As the protective layer wears away, the bones begin to rub against one another. That friction causes pain, inflammation, and stiffness, and over time, it can lead to significant joint damage. In older adults, this typically happens as a result of gradual aging. In younger patients, something else may be driving it.
Why Does Shoulder Arthritis Develop in Younger Patients?
When I evaluate a younger patient with shoulder arthritis, one of my first goals is to understand what caused the joint breakdown in the first place. There is almost always a contributing factor, and in many cases, several working together.
Prior Injury or Trauma
One of the most common causes I see is post-traumatic arthritis. This occurs when a previous injury, such as a shoulder fracture or dislocation, damages the cartilage or disrupts the mechanics of the joint. Even if the injury seemed to heal well at the time, the long-term effects can set the stage for arthritis years or even decades later.
For example, a fracture of the humeral head can leave the joint surface irregular. That subtle irregularity acts a bit like a rough patch on an otherwise smooth road, and it causes accelerated wear on the surrounding cartilage over time. Similarly, repeated shoulder dislocations can chip away at the cartilage and bone, gradually destabilizing the joint and setting arthritis in motion.
Repetitive Overuse
Athletes and individuals with physically demanding jobs often accumulate stress on the shoulder joint over many years. Baseball pitchers, swimmers, weightlifters, and overhead workers may place unusually high loads on the shoulder repeatedly, year after year. This kind of cumulative stress may accelerate cartilage breakdown.
Inflammatory Conditions
Certain systemic conditions can directly attack the cartilage and soft tissues of the shoulder. Rheumatoid arthritis is one of the most well-known examples. It’s an autoimmune condition in which the body’s immune system mistakenly targets its own tissues, including the cartilage lining of the joint. Other inflammatory conditions may also affect the shoulder and contribute to early arthritis.
Avascular Necrosis
Avascular necrosis (AVN), sometimes called osteonecrosis, is a condition in which the blood supply to the bone is interrupted, causing bone tissue to die. When this affects the humeral head, the bone can collapse and the joint surface becomes irregular, leading to rapid cartilage breakdown. AVN in the shoulder may be linked to high-dose corticosteroid use, excessive alcohol consumption, prior trauma, or certain blood disorders. It’s not an everyday diagnosis, but in younger patients with shoulder arthritis, it’s one of the possibilities a specialist will want to consider.
Primary Osteoarthritis in Younger Adults
Primary osteoarthritis, the “wear and tear” variety most often associated with aging, can occasionally develop in younger adults, particularly those with a genetic predisposition. While it’s less common in this age group, it does happen, and it may present without any clear triggering injury or underlying condition. In these cases, the cartilage simply breaks down earlier than expected.
Recognizing the Symptoms
Shoulder arthritis in younger patients can sometimes be dismissed or misdiagnosed simply because people don’t expect this diagnosis at a young age. It’s worth knowing what to watch for.
Pain is typically the most prominent symptom. It may start as an ache that shows up during certain activities and gradually becomes more constant over time. Many patients notice the pain worsening with activity and improving somewhat with rest, though as the condition progresses, even rest may not fully provide relief. Night pain is also common and can begin to disrupt sleep.
Stiffness is another common finding. You might notice that your shoulder no longer moves through its full range the way it used to. Getting dressed, reaching behind your back, or lifting your arm overhead may feel restricted or require extra effort. This loss of motion can often feel like it sneaks up on you gradually.
Crepitus, a grinding, clicking, or crackling sensation inside the joint, can occur as cartilage wears away and the bone surfaces become rougher. Some patients describe it as a feeling that something is “catching” inside the shoulder during movement. In more advanced cases, a sense of weakness or instability may also develop, either from pain inhibiting normal muscle use or from associated damage to surrounding structures like the rotator cuff.
Because these symptoms can overlap with many other shoulder conditions, a thorough evaluation by an experienced shoulder specialist is important before drawing any conclusions.
Getting a Diagnosis
When I see a patient who may have shoulder arthritis, the evaluation begins with a detailed history. I want to know about any past injuries, prior surgeries, relevant health conditions, and medications. I’ll ask about what makes the pain better or worse, how long it has been going on, and how it’s affecting daily life and activities.
A physical examination follows. I assess range of motion, strength, areas of tenderness, and any signs of instability or other concurrent conditions. This hands-on evaluation helps narrow things down considerably before we even look at imaging.
X-rays are typically the starting point and can reveal joint space narrowing, bone spurs, and other hallmarks of arthritis. CT scans offer a more detailed three-dimensional view of the bone and are particularly useful when I need to evaluate bone loss, deformity, or the anatomy of the glenoid in detail. MRI may be ordered to assess the health of the rotator cuff, labrum, and other soft tissues that might be involved alongside the arthritis.
Treatment Options
Treating shoulder arthritis in younger patients requires careful thought. The goal isn’t just to reduce pain right now. We also have to think long-term. That means preserving as much of the natural joint as possible, maintaining function for an active lifestyle, and, if surgery eventually becomes necessary, choosing an approach that makes sense for someone who may live with their shoulder for many more decades.
Non-Surgical Management
For many younger patients, non-surgical treatment is the right starting point. The goal here is to manage symptoms, slow progression where possible, and maintain quality of life. Several approaches may help, and they often work best in combination.
Physical therapy commonly plays an important role. A well-designed program focuses on maintaining mobility, strengthening the muscles that support the shoulder, and reducing stress on the joint during daily activities and exercise. Many patients find that a consistent, progressive therapy program makes a meaningful difference in how their shoulder feels and functions day to day.
Anti-inflammatory medications may help manage pain and swelling. Your doctor might also recommend a corticosteroid injection into the joint to provide relief during a particularly painful flare. There has been much recent interest in the use of ‘biologics’ for injection including platelet-rich plasma (PRP), various stem cell derivatives. I have studied the impact of these in the laboratory and have also published on this topic. Unfortunately, the current scientific data and clinical results continue to be inconsistent at this time and as a result, these therapies are not covered by insurance and can require significant cost to the patient.
Activity modification is also part of the picture. This doesn’t necessarily mean giving up the activities you enjoy, but it may mean adjusting how you approach them. Consider avoiding certain high-impact movements, pacing yourself differently, or using better technique to reduce joint stress over time.
Surgical Options
When non-surgical treatment no longer provides adequate relief, surgery may become appropriate. The surgical options available depend on the type and severity of the arthritis, the condition of surrounding structures like the rotator cuff, and your individual goals and activity level.
For younger patients with earlier-stage arthritis and relatively preserved joint surfaces, shoulder arthroscopy may be a reasonable option, called “comprehensive arthroscopic management” or a CAM procedure. During this minimally invasive procedure, I can remove loose cartilage fragments, address bone spurs, release tight soft tissues, and treat other contributing problems and ‘pain-generators’ within the joint. Arthroscopy doesn’t eliminate the arthritis, but it may reduce pain and improve motion in appropriately selected patients.
In patients with more significant cartilage loss but a healthy rotator cuff, a total shoulder replacement may eventually be considered. In younger patients specifically, the choice of implant, technique, and surgical approach requires particularly careful consideration. Robotic-assisted shoulder replacement may support more precise implant positioning. Some newer implant designs are better suited for more active patients where loosening may be a concern, such as the InSet® Total Shoulder System.
In cases where both arthritis and significant rotator cuff damage are present, a reverse shoulder replacement may be the more appropriate solution. This procedure redesigns the mechanics of the joint, allowing the deltoid muscle to take over much of the work that a damaged rotator cuff can no longer perform. However, this device is used very selectively in higher-demand young patients.
Summary
While it can feel discouraging to receive a diagnosis of arthritis at a young age, treatment options are available that may help you manage symptoms and protect your shoulder over the long term. Understanding what caused the arthritis, how advanced it is, and what your personal goals are all shape the treatment plan. In my experience, patients often do best with an accurate diagnosis, an individualized approach, and a thoughtful commitment to the treatment process with the right care team.
Frequently Asked Questions
Can shoulder arthritis really happen in your 30s or 40s?
Yes, it can. While shoulder arthritis is more commonly associated with older adults, it does develop in younger patients, often as a result of prior injury, inflammatory conditions, overuse, or other underlying factors.
Is surgery inevitable if I have shoulder arthritis at a young age?
Not necessarily. Many younger patients manage their arthritis effectively with non-surgical treatment for months or even years. Whether and when surgery becomes appropriate depends on how the arthritis progresses, how much it affects daily life and function, and how well non-surgical options continue to provide relief.
What’s the difference between arthritis caused by an old injury versus regular wear and tear?
Post-traumatic arthritis, the type linked to a prior injury, tends to develop earlier in life and can involve more complex joint anatomy. Primary osteoarthritis typically develops more gradually with age. The symptoms may look similar, but understanding the cause matters because it influences both the treatment approach and the surgical planning if surgery eventually becomes necessary.



