The shoulder is one of the most complex and mobile joints in the human body. This range of motion allows us to perform countless daily activities, from reaching for a high shelf to throwing a ball. However, this complexity and constant use also make the shoulder susceptible to wear, tear, and injury. A question that frequently arises for those experiencing persistent shoulder pain is: Can you get arthritis in your shoulder? The definitive answer is yes. In this post, we’ll break down what that means, how it develops, and what treatment options look like.
Key Takeaways
- Arthritis commonly affects the two main joints of the shoulder: the glenohumeral (main shoulder joint) and the acromioclavicular (AC) joint.
- The five most common types of shoulder arthritis are osteoarthritis (OA), rheumatoid arthritis (RA), post-traumatic arthritis, rotator cuff tear arthropathy, and avascular necrosis (AVN).
- Common signs include deep, aching pain, stiffness, a grinding or clicking sensation (crepitus), and a progressive loss of range of motion.
- A specialist typically diagnoses shoulder arthritis through a physical examination, patient history, and imaging tests.
The Anatomy of Shoulder Arthritis: Where Does It Occur?
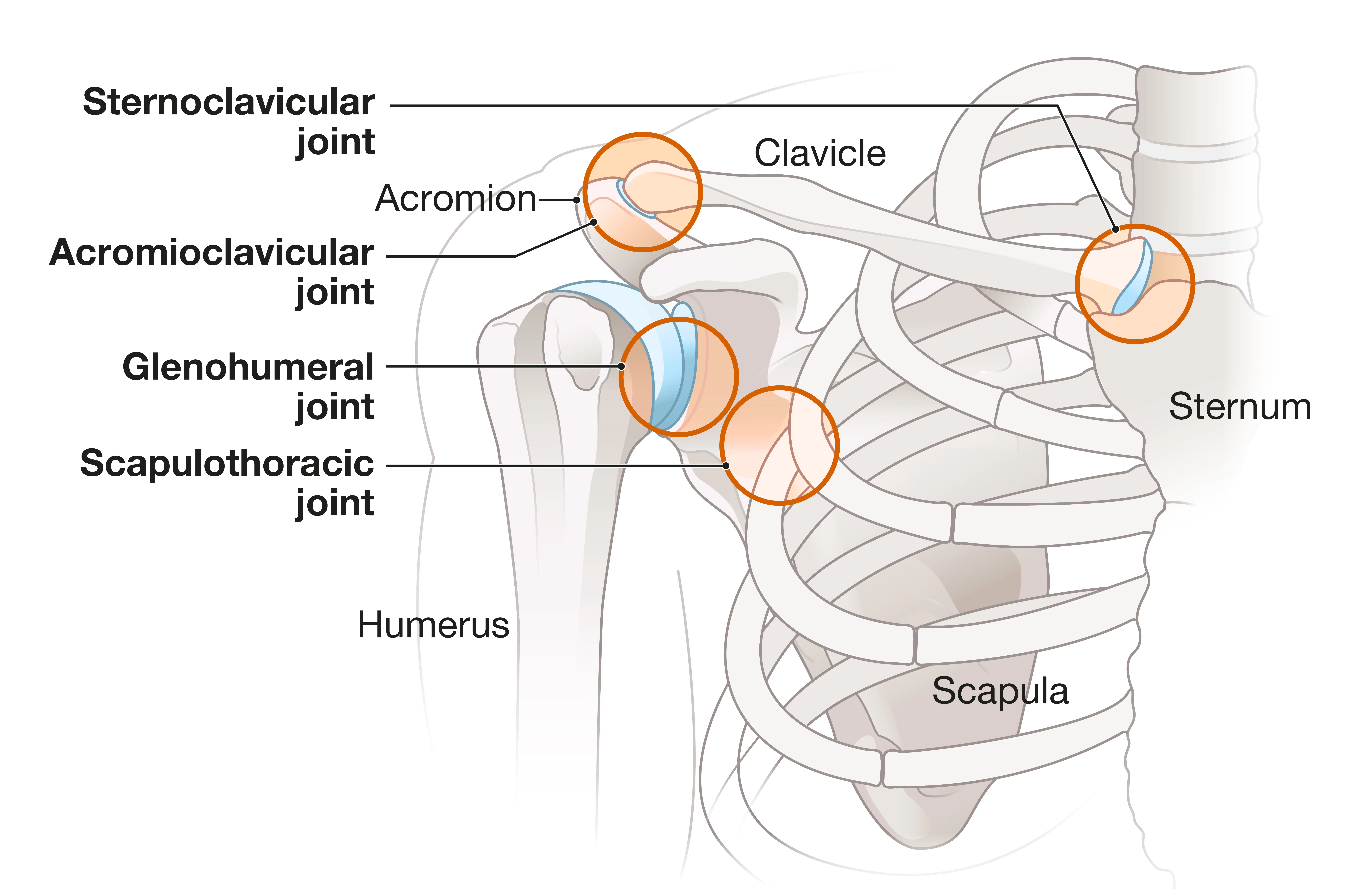
The shoulder is not just one joint; it is a complex of several joints, muscles, and tendons working in harmony. Arthritis primarily targets two specific joints within this complex: the glenohumeral joint and the acromioclavicular (AC) joint.
1. The Glenohumeral Joint
This is the main ball-and-socket joint of the shoulder. The humerus (upper arm bone) has a rounded head that fits into the glenoid (a shallow socket on the shoulder blade, or scapula). Both the ball and the socket are covered with a smooth, slippery tissue called articular cartilage. This cartilage allows the bones to glide effortlessly against each other during movement.
2. The Acromioclavicular (AC) Joint
The AC joint is located at the top of the shoulder. It is the connection point between the acromion (part of the shoulder blade) and the clavicle (collarbone). This joint is much smaller than the glenohumeral joint, but it is important for shoulder function.
Types of Shoulder Arthritis
While many people associate arthritis with simple aging, the condition is far more nuanced. Several distinct types of arthritis can affect the shoulder, each with its own underlying cause and progression.
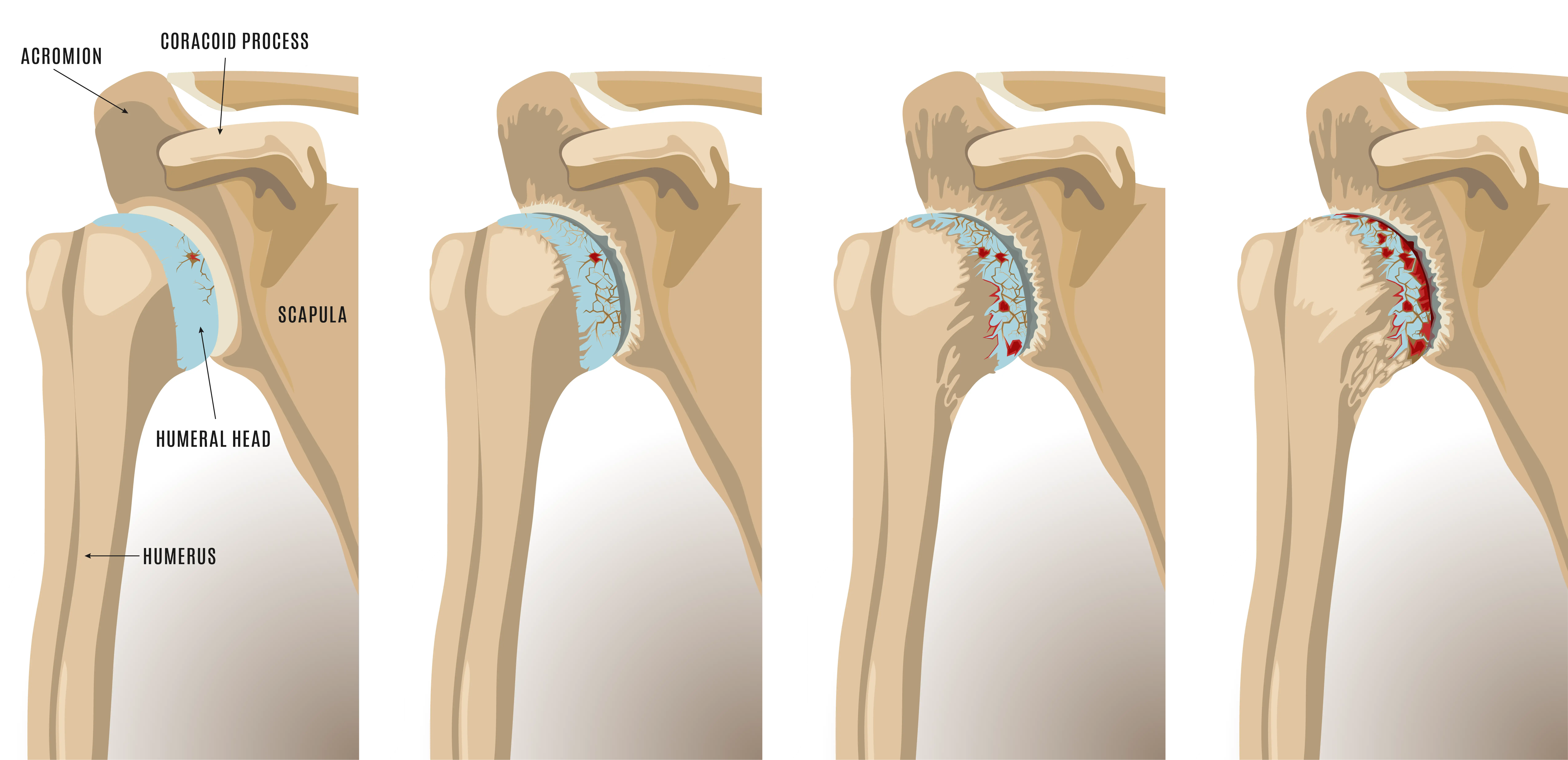
Osteoarthritis (OA)
Osteoarthritis is the most common form of shoulder arthritis. It may be referred to as “wear-and-tear” or degenerative arthritis.
- Cause: OA develops as the protective articular cartilage on the ends of the bones gradually deteriorates. This process is often linked to aging, genetics, and long-term mechanical stress on the joint.
- Progression: As the cartilage thins, the bones begin to rub against each other. The body may attempt to repair the damage by growing small, bony projections called osteophytes or bone spurs. These spurs can further restrict movement.
- Affected Joints: OA most frequently affects the glenohumeral joint, but it is also a common cause of pain in the acromioclavicular (AC) joint.
- Symptoms: Pain generally worsens with activity and improves with rest. Patients frequently report a deep, aching sensation and a grinding or clicking noise when moving the arm.
Rheumatoid Arthritis (RA)
Rheumatoid arthritis is a systemic, autoimmune disease. This means the body’s own immune system mistakenly attacks the healthy tissues lining the joints.
- Cause: The immune system targets the synovium, the membrane that surrounds the joint and produces lubricating fluid. This causes inflammation, which can eventually destroy the articular cartilage and erode the underlying bone.
- Progression: RA typically affects both shoulders simultaneously, as well as other joints throughout the body. The inflammation can lead to joint damage and deformity if left untreated.
- Symptoms: Unlike OA, RA pain is often worse after periods of rest, such as first thing in the morning. Swelling, warmth, and tenderness are potential signs of an RA flare-up.
Post-Traumatic Arthritis
This type of arthritis develops after a significant injury to the shoulder.
- Cause: Any severe trauma, such as a fracture of the humerus or glenoid, or a serious shoulder dislocation, can damage the articular cartilage. Even if the injury is treated effectively, the initial damage may disrupt the joint’s mechanics.
- Symptoms: The symptoms are very similar to osteoarthritis, including pain and stiffness, but the patient’s history of a major shoulder injury can be a key distinguishing factor.
Rotator Cuff Tear Arthropathy
This is a severe and complex shoulder condition that combines two major problems: a massive, long-standing rotator cuff tear and advanced arthritis.
- Cause: A large, chronic tear in the rotator cuff tendons causes the head of the humerus to shift upward and rub against the acromion. This abnormal positioning and friction destroy the articular cartilage.
- Progression: The combination of a non-functional rotator cuff and a severely damaged joint can lead to a condition where the shoulder is both painful and extremely weak. Patients may struggle to lift their arm at all.
- Treatment Consideration: This specific type of arthritis may require a specialized surgical solution, such as a reverse shoulder replacement.
Avascular Necrosis (AVN)
Avascular necrosis, also known as osteonecrosis, is a condition where the bone tissue dies due to a lack of blood supply.
- Cause: The blood supply to the head of the humerus may be interrupted by a severe fracture, certain medical conditions, and some medications.
- Symptoms: Pain from AVN often begins as a deep ache that occurs with activity, but it typically becomes more persistent over time.
Recognizing the Signs: Symptoms of Shoulder Arthritis
The symptoms of shoulder arthritis frequently begin subtly and worsen gradually over time. Recognizing these early signs is important for seeking timely medical evaluation. While the specific presentation can vary depending on the type of arthritis and the joint affected, several common symptoms regularly present in patients.
Pain Characteristics
Pain is the most consistent symptom. It is usually described as a deep ache within the joint. In glenohumeral arthritis, this pain is often felt in the back of the shoulder and may travel down the arm. In AC joint arthritis, it tends to stay at the top of the shoulder.
Stiffness and Loss of Motion
As cartilage wears down and bone spurs form, the joint space narrows, making the shoulder increasingly stiff. Patients often notice difficulty with everyday tasks like fastening a seatbelt or combing their hair. A grinding or clicking sensation, known as crepitus, is also common and occurs when rough bone surfaces rub together during movement.
Weakness and Instability
In more advanced cases, particularly with rotator cuff tear arthropathy, the shoulder may feel weak. Although less common, severe joint damage can sometimes create a sense of instability or the feeling that the shoulder might “give out.”
The Diagnostic Journey: Confirming Shoulder Arthritis
The diagnostic process is a systematic approach that combines a thorough patient history, a physical examination, and advanced imaging studies.
Patient History and Physical Examination
Your doctor may begin by asking detailed questions about the symptoms. A history of previous shoulder injuries, systemic diseases like rheumatoid arthritis, and family history are all generally relevant. During the physical examination, the doctor may assess range of motion, gently press on different areas of the shoulder joint for tenderness, and perform specialized tests to evaluate strength and stability.
Imaging Studies
Imaging may be used to support the diagnosis and determine the severity of the arthritis. Standard X-rays may show the bones and can reveal classic signs of arthritis, including joint space narrowing and osteophytes. An MRI provides detailed images of soft tissues, such as the rotator cuff tendons. A CT scan is often used to assess the bone structure in greater detail, particularly when planning for a complex surgical procedure.
Treatment Options: From Conservative Care to Advanced Surgery
The treatment for shoulder arthritis is highly individualized and depends on the type of arthritis, its severity, the patient’s age, and their activity level.
Non-Surgical Management
For many patients, especially in the early stages of arthritis, non-surgical treatments may be used to manage pain and maintain function.
Lifestyle Modifications and Activity Changes
Making small adjustments to daily habits can reduce irritation in the joint. Patients may be advised to avoid activities that reliably trigger pain, such as heavy lifting or repetitive overhead motion. Low-impact exercises like walking, swimming, or using an elliptical may help keep the shoulder mobile without overloading it.
Medications and Injections
Over-the-counter medications may offer relief. NSAIDs (such as ibuprofen or naproxen) can help reduce pain and inflammation, while acetaminophen may ease discomfort for those who cannot take anti-inflammatories. Corticosteroid injections may reduce inflammation and provide temporary pain relief for some patients.
Physical Therapy
A structured physical therapy program can maintain or improve range of motion and strengthen the muscles that support the shoulder, including the rotator cuff and scapular stabilizers. A therapist may guide patients through gentle stretching and targeted strengthening exercises tailored to their symptoms.
Surgical Management
When non-surgical treatments no longer provide adequate relief, or when the arthritis is advanced, surgical intervention may be the most appropriate next step. The goal of surgery is to relieve pain and restore function.
Arthroscopy
Shoulder arthroscopy is a minimally invasive procedure performed through tiny incisions using a small camera and specialized instruments. In the early stages of arthritis, a surgeon may use arthroscopy to clean out the joint, remove loose cartilage fragments, release the capsule to improve range of motion, and carefully trim any bone spurs.
Arthroscopy may also be used to address isolated AC joint arthritis by removing a small portion of the end of the collarbone, a procedure called distal clavicle excision. Creating this space helps prevent the bones from rubbing together, which can reduce pain and improve shoulder mechanics.
Total Shoulder Arthroplasty (Anatomic Total Shoulder Replacement)
During a total shoulder replacement procedure, both sides of the joint are resurfaced. The humeral head is replaced with a metal ball attached to a stem placed inside the upper arm bone, and the socket is fitted with a smooth plastic component. This approach is typically recommended for severe osteoarthritis or post-traumatic arthritis when the rotator cuff tendons remain healthy and intact.
Reverse Total Shoulder Arthroplasty
Reverse total shoulder replacement is designed for patients who have rotator cuff damage, especially those with rotator cuff tear arthropathy. Instead of recreating the shoulder’s native anatomy, the positions of the ball and socket are reversed: a metal ball is placed on the glenoid, and a plastic socket is attached to the humerus. This change shifts the mechanics of the joint, so patients may rely on the deltoid muscle rather than the injured rotator cuff to lift the arm.
Summary
The answer to the question, “Can you get arthritis in your shoulder?” is yes. However, with modern orthopedic care, patients have access to a wide spectrum of treatment options, from conservative management strategies to advanced surgical techniques like total and reverse shoulder replacement. By understanding the specific types of arthritis, recognizing the symptoms, and partnering with a dedicated shoulder specialist, you can take proactive steps toward managing your pain and restoring your mobility.
Frequently Asked Questions
How is shoulder arthritis different from a rotator cuff tear?
They are distinct conditions, but they can be related. A rotator cuff tear involves damage to the tendons and muscles that stabilize and move the shoulder. Arthritis involves the deterioration of the joint cartilage. However, a massive, long-standing rotator cuff tear can cause a form of arthritis called rotator cuff tear arthropathy.
What is the recovery time like after a total shoulder replacement?
Recovery from a total shoulder replacement is a structured process, and timelines may vary between patients. The arm is typically immobilized in a sling for the first few weeks. Formal physical therapy usually begins soon after surgery. While pain relief is often experienced sooner, achieving strength and range of motion can take anywhere from four to six months or longer. Your surgeon and physical therapist will guide you through a personalized recovery timeline.
What activities should I avoid if I have shoulder arthritis?
Activities that consistently provoke pain, especially heavy lifting, repetitive overhead motion, or forceful pushing/pulling, might aggravate symptoms. Your specialist or physical therapist can help tailor activity recommendations based on your condition and goals.



